A Special Nail for a Floating Kneecap
Leiloni Wonch adopted Birdie, a playful mixed breed dog, from a local animal shelter. Because she was just about 10 months old, healthy, and active, Leiloni wasn’t immediately concerned when Birdie developed a limp in her right hind leg.

Leiloni first noticed the limp after Birdie got her leg stuck under her seatbelt during a car ride. She kept a watchful eye on Birdie’s gait, and was relieved when it disappeared a few days later. But the limp returned, and then began switching from one rear leg to the other.
“I thought it was growing pains, to be honest,” Leiloni says. “I watched the limp progress for about a month because I thought it might go away on its own.”
When Birdie didn’t show signs of improvement, Leiloni scheduled an orthopedic consultation at the MSU Veterinary Medical Center. “I brought Birdie directly to MSU because I trust you guys the most,” Leiloni says. “I knew that if anything had to be done that I’d be coming to MSU, so I figured I would start here.”
They met with orthopedic surgeon Loic Déjardin, DVM, MS, DACVS, DECVS, who diagnosed Birdie with patellar luxation, a congenital condition that causes the patella, or kneecap, to slide out of its normal position in a groove at the bottom of the femur, or thigh bone. The condition is sometimes called a floating kneecap, and was unrelated to the seatbelt incident. Without surgery, this painful condition continues to degenerate, erodes cartilage, causes arthritis, and can result in permanent lameness. As with about half the dogs with this condition, both of Birdie’s knees were affected. Her first knee was operated on the week following her first appointment.
Traditionally, to repair patellar luxation, the surgeon cuts the femur in two places, corrects its deformity, and stabilizes it with a steel plate. Déjardin uses distal femoral osteotomy (DFO), a procedure that repairs the femur with only one cut to the bone. Instead of a plate, a locking nail is inserted into the bone. Déjardin developed the nail, called the iLoc, in 2003.
The procedure is less invasive, heals more quickly, and is less expensive than the traditional surgery. Risk of infection is reduced because the locking nail is inserted into the bone instead of being attached externally. It is uncommon for the condition to recur after surgical correction.
Birdie is recovering exceptionally well. Within a week of surgery, she was bearing weight on her leg. When it is fully healed, the second knee will be repaired.
To achieve a quick and full recovery, Birdie comes to the Animal Rehabilitation Center for physical therapy. “My experience with the hospital, Dr. Déjardin, and all the other people involved with Birdie’s recovery has been very positive,” Leiloni says.
Birdie is expected to make a full recovery and be as lively as before.
Helping Jake
The many options for diagnostic imaging at the VMC were a significant boon to Jake, a nine-year-old Labrador retriever, who was referred to MSU’s Orthopedic Surgery Service because of his continuous right forelimb lameness.
Despite medical management of the lameness – weight management, anti-inflammatory medication, chondroprotective agents, and underwater treadmill rehabilitation – his condition had become progressively worse.
Radiographs of the right and left shoulders showed calcification of the tendon of insertion of the supraspinatus muscle (part of the rotator cuff), and the right elbow showed severe degenerative joint disease (DJD).
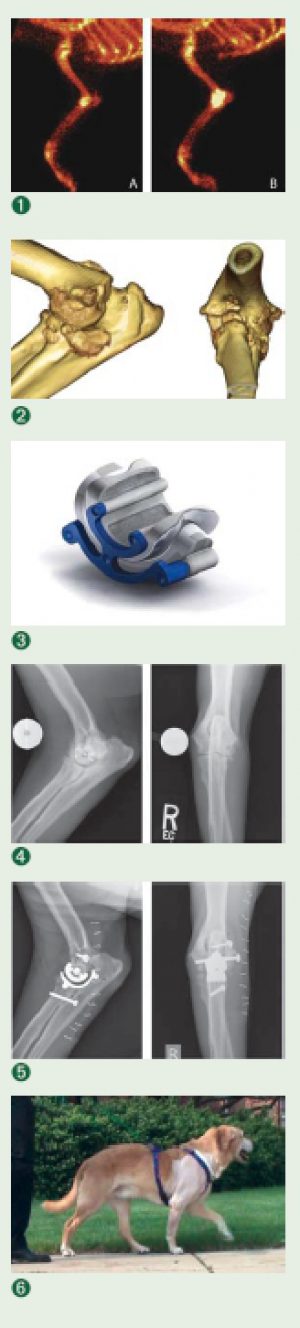
Despite these abnormal radiographic findings in the right elbow and shoulder, Jake showed no pain when his right elbow was manipulated. Orthopedic surgeon Dr. Jennifer Au ordered soft tissue and bone nuclear scan in an attempt to better localize the origin of the right forelimb lameness. [Fig.1]
When the nuclear scan (also called scintigraphy) showed that the right elbow was the most likely source of Jake’s condition, Au ordered a CT scan to identify any bone fragments that could be surgically removed from the elbow joint. The CT scan confirmed the diagnosis of severe right elbow DJD, but no fragment was seen. [Fig. 2]
In October 2007, the time of Jake’s first visit to the VMC, the best option for him was continued medical management, but six months later a new option became available – a cementless total elbow prosthesis (TATE Elbow System from BioMedtrix) [this option was described in "New Elbow Prosthesis Available At VMC"][Fig. 3]. Jake’s owners were willing to enroll him in the clinical phase of this new elbow replacement design.
Dr. Loic Dejardin, orthopedic surgeon, ordered preoperative elbow radiographs to determine the appropriate size of the prosthesis [Fig. 4], and he and his colleagues, Dr. Reunan Guillou (a surgery resident at the VMC) and Randy Acker (inventor of the prosthesis), performed surgery on April 28. They encountered no complications during the surgical procedure, and postoperative radiographs showed adequate placement of the prosthesis. [Fig 5] There was significantly improved range of motion in the right elbow both during and after the surgery.
Because this prosthesis was designed with a minimally invasive surgical approach in mind, they only needed to place a slight padded bandage for the first 24 hours. Jake was already bearing significant weight on his right forelimb 24 hours postoperatively, and at 12 weeks after surgery, he is doing better than before surgery. [Fig. 6]
For more information about this total elbow replacement at MSU, contact Dr. Loic Dejardin.
