As protectors of animal health, veterinary professionals at the Michigan State University Veterinary Medical Center are tasked with making tough decisions and providing the best possible care to their patients and clients. These Spartans give animals who appear to be on death’s door not only a fighting chance at survival but a continuation of life—even in unthinkable situations. From the perspective of the team behind the scenes, Dr. Matt Beal recalls the intense, harrowing, emotional tale of a young Husky who was shot and left for dead, and thanks the critical workers who saved his life.

In the afternoon of May 24, 2022, the Emergency and Critical Care Medicine Service (ECCM) at MSU was presented with King, a young Husky who had been shot in the abdomen and found collapsed in a drainage ditch. On presentation, he had no palpable or measurable blood pressure, was unresponsive, and had a temperature too low to read. He was hemorrhaging and his life was on the line. “From the moment he hit the table, everyone pitched in to give King the best chance at a positive outcome,” says Beal.
The mission to save King’s life began as soon as he arrived at MSU. Front-of-house triage students immediately helped get him back to the resuscitation station where ECCM faculty, residents, nurses, veterinary assistants, and students then hit the ground running; they worked to get vascular access for resuscitation, got monitors going, set up fluids, prepped necessary medications, advocated for pain meds and antibiotics, etc. Whatever was needed, the ECCM team did it.

While the team battled to save King’s life in the Small Animal Intensive Care Unit (ICU), Dr. Caitlin Kupiec, former rotating intern for the MSU Small Animal Clinic, handled the face-to-face consent and preparation of the clients. “It’s so hard to put into words how amazing everyone at MSU was, from the moment we arrived with King,” says King’s owner.
Back in the Small Animal ICU, Dr. Elizabeth Gregory, and Dr. Cameron Henke, both residents for the MSU Small Animal ECCM, were in the trenches; from resuscitation and stabilization to trauma management and urgent tests, these veterinary residents wasted no time—because time wasn’t something King had. “They guided all aspects of King’s diagnostics and management efficiently and accurately,” says Beal.
From the ICU station to the CT table in Diagnostic Imaging, King was quickly rushed over on a gurney. “The Diagnostic Imaging team cleared the room and rushed King to the front of the queue, a critical move as we had to determine the extent of his injuries and we had to do it fast,” says Beal. A swift read revealed several perforations along the track of the bullet in the small intestine and a femoral fracture (thigh bone) where the bullet impacted.
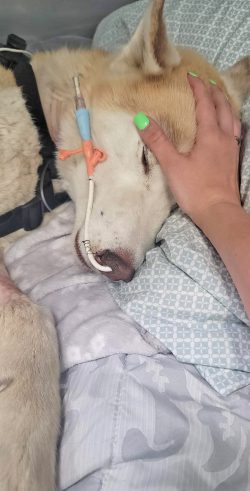
While King was in Diagnostic Imagining, Dr. Thibault of the Anesthesia and Pain Management Service was on standby for whatever King needed. “I told him we had a dog that we’d be bringing soon and that it was bad,” recalls Beal. Alongside Anesthesia, the operating room nurses prepped the surgical suite before the team even definitively knew what King would need surgery for—or if he would even make it to surgery. “They did this so that no time would be wasted because we didn’t have time to waste,” adds Beal.
King had a severe and life-threatening hemorrhage in his abdomen. He received more than half his blood volume in transfusions (including a rapid infusion of 2u of blood and 2u plasma over less than 30 minutes) and more than two-and-a-half times his blood volume in other resuscitation fluids. “Veterinary Nurse Rose Wahl keeps our blood bank prepped for these kinds of cases. In few facilities can you run to the blood bank and grab what the patient needs without causing a huge shortage or worse. And there was more if we needed it,” says Beal.
Once he was resuscitated, the immediately life-threatening issue was King’s multi-perforated small intestine (jejunum). So, into emergency surgery King went, where the MSU Soft Tissue Surgery team, led by Dr. Maureen Spinner (formerly Jay), repaired the perforated portions of King’s small intestine, flushed his abdomen out, and established drainage. A life-saving surgery, this fast-acting treatment kept King’s infection from spreading and potentially progressing to septic shock, an often-fatal condition.
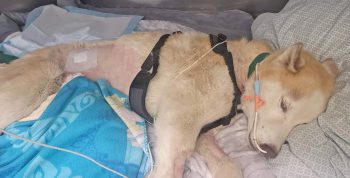
King came out of anesthesia and was eventually taken off pressors, the medication that treated his critically low blood pressure. The team spent the evening sorting out his various conditions and setting him up for the days ahead. He was heavily monitored, and the road ahead was assumed to be bumpy. The team knew they would need to manage King’s femoral fracture in the future, as the bullet passed through his abdomen while it was on its way to his femur. “But that’s a surgery for another day,” comments Beal.
Long days and weeks would follow the first long, long night in ECCM, not only for King but also for the team who fought around the clock to keep him alive. “We could not be more grateful for the team who worked on King and took care of him,” says King’s owner. “No words can come close to describing how we feel about this team. Because of them, he’s going to make it. Our boy is going to make it!”
“With few exceptions, at almost any other facility in the world, this dog likely would not have made it. I had times during the evening King was admitted when I thought he would die. He currently still has a long journey ahead of him, but he’s in the fight, thanks to so many people here at the Hospital,” says Beal.
*King spent three weeks in the Hospital. He underwent three surgeries, countless procedures, and a near-death experience. Today, he’s back home with his owners. His life isn’t the same as it was before he was shot, but he’s alive. Stay tuned for part two of King’s story.
