By Julie Strachota, DVM, MS, clinician for the MSU Theriogenology Service; Ashley VanderBroek, DVM, DACVS-LA, clinician for the MSU Large Animal Surgery Service
Featuring Dr. Meredith Hare-Drubka, second-year resident for the MSU Large Animal Medicine Service; Dr. Jackie Willette, second-year resident for the MSU Large Animal Surgery Service; Shelbe Vollmer, MSU DVM Class of 2021
History and Presentation
Cookie, a 12-year-old Saddlebred mare, was presented to Michigan State University Veterinary Medical Center’s Large Animal Emergency Service for colic and possible abortion. Cookie’s owners found her colicking in her stall in the morning with a portion of her placenta and some blood on the stall floor but no foal. Cookie was suspected to be 30 days from her due date and had foaled in the past without complications. Cookie was given a dose of oral Banamine on the farm and brought to MSU for further evaluation.
On presentation, Cookie was bright, alert, and responsive. Her mucous membranes were pale pink with a capillary refill time of fewer than two seconds. Her eyes and nose were clean and clear of debris with no discharge, but her sclera appeared injected. Cardiopulmonary auscultation was unremarkable with no appreciable arrhythmias, murmurs, crackles, or wheezes. Gastrointestinal borborygmi were present in all abdominal quadrants. Digital pulses were within normal limits and the mare was fully weight-bearing on all limbs at the walk. Cookie was not straining and did not appear to be having active uterine contractions.

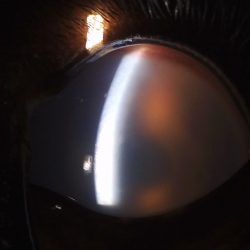
To assess fetal viability, transabdominal ultrasonography was performed. Fetal heartbeat and movement were not appreciable. A transrectal examination was performed to assess fetal presentation, position, and posture as well as evaluation of uterine tone, cervical relaxation, and any appreciation of fetal movement upon stimulation. No fetal movement was appreciable, the cervix was dilated, and no fetal extremities were noted within the pelvic inlet.
To further evaluate the fetal presentation, position, and posture, a vaginal examination was performed following aseptic preparation of the perineum. The fetus was identified in anterior, longitudinal, dorsosacral presentation with flexion of both carpi and left lateral flexion of the head and neck.
On admission, a venous blood gas revealed mild hyperlactatemia at 3.8 mmol/L (RR: 0.3-1.1 mmol/L), but all other bloodwork was within normal limits.
Diagnosis
Based on bloodwork, reproductive evaluation, and ultrasound, Cookie was diagnosed with dystocia due to malposture of a deceased fetus.
Treatment and Outcome
After discussing possible treatment options with Cookie’s owner, it was decided to attempt a vaginal delivery and not rush to cesarean section since the fetus was deceased.
Cookie was sedated and an assisted vaginal delivery was attempted standing in stocks. Both carpi were extended but the head and neck remained laterally flexed despite multiple manipulations. It was decided to proceed with a controlled vaginal delivery at that point.
Cookie was placed under general anesthesia and positioned in left lateral recumbency with her hind limbs hoisted vertically. The fetus was repositioned within the uterus so that the head and both forelimbs were extended. A deceased fetus was then delivered with the assistance of obstetric chains. The corneas of the fetus were cloudy with no signs of emphysema or sloughing of the fetus’s hair. This suggested that the fetus had been dead for at least 6 hours. The amnion and a portion of the necrotic placenta were delivered with the fetus, but the entire gravid left horn remained firmly attached. A thorough reproductive examination was performed to rule out the presence of a twin and to assess the uterine and vaginal mucosal integrity, which was unremarkable.
The umbilical vessel water infusion technique was attempted to facilitate the removal of the remaining placenta but was unsuccessful. During this process, the uterus began to partially prolapse, so the procedure was discontinued, and the uterus was repositioned. Cookie recovered uneventfully from anesthesia.
Cookie was put on intravenous antibiotics, anti-inflammatory medication, and oxytocin. Cryotherapy of her front hooves was attempted but she was not amendable to this therapy. Uterine lavage was completed twice daily to help remove the retained fetal membranes, address the uterine contamination, and prevent secondary endotoxemia.
Throughout Cookie’s week-long hospitalization, full physical exams were performed every six hours. On the first morning of hospitalization, Cookie’s mucous membranes were mildly injected but normalized within 12 hours. A complete blood count was submitted at this point and revealed a moderate leukopenia at 2,800 WBC/uL (RR 4,700-9,500 WBC/uL) with left shift (600 band neutrophils/uL) and toxic change. Her vital parameters stayed within normal limits and her digital pulses remained normal. Cookie did not develop any signs of laminitis throughout her stay at MSU. To promote uterine contractions, Cookie was hand walked every 6 hours while hospitalized.
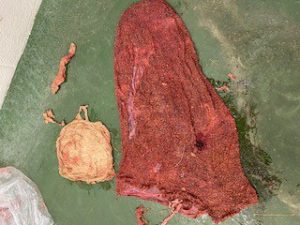
Four days post-admission, the retained fetal membranes were successfully passed. Uterine lavage was performed two more times to ensure the fluid return was relatively clear. Once the retained fetal membranes were passed, Cookie was switched from intravenous to oral antibiotics and she remained bright with normal vital parameters throughout the remainder of her hospitalization.
Six-months post-admission, Cookie’s owners report her to be doing well with hopes of rebreeding her next year. It was recommended that she receive a breeding soundness examination prior to being bred in the 2022 breeding season.
Comments
Equine dystocia is always an emergency. Quick diagnosis and experience are key to a successful outcome for the mare and foal. In the mare, stage 2 of parturition, as defined by the rupture of the chorioallantoic membrane, should last no more than 30 minutes. Failure of notable progression of the fetus within 15 minutes warrants immediate veterinary intervention.
When assessing a mare with dystocia, a thorough history and physical exam are necessary to decide how to handle the dystocia. Aseptic technique should be used when preparing the perineum for vaginal examination. Copious amounts of obstetrical lubricant are recommended during the vaginal exam and during manipulation of the fetus. The position of the fetus is described using the following terms: presentation, position, and posture. Presentation is the portion of the fetus entering the pelvic canal first (anterior, posterior, or transverse). Position describes the relationship of the dorsum of the fetus to the mare’s pelvis (dorsosacral, dorsopubic, or dorsoilial). Posture is the location of the fetal extremities in relation to itself. Postural abnormalities such as a flexion of the head and neck or limbs are the most common causes of dystocia in the mare.
In the presented case, vaginal delivery was attempted as the fetus was deceased. We confirmed this by ultrasound and palpation, but with the amount of placenta already passed prior to presentation, the fetus had been in a hypoxic environment for too long. If the fetus was alive, controlled vaginal delivery would have been performed for a maximum of 15 minutes prior to moving her into the surgical suite for a cesarean section.
Time is critical when dealing with a dystocia. It is important for clients to understand the urgency of this emergency and to have a plan prior to foaling to increase the chance of a successful outcome for the mare and foal.