History and Presentation
Lilah, an 11-week-old Berniedoodle was presented to the MSU Orthopedic Surgery Service for evaluation of a right tibial fracture diagnosed by her family veterinarian. At approximately 8:00 a.m. the morning that Lilah was presented; she was playing as normal with her housemate (a 90 lb. Bernese Mountain Dog). Her owner heard a yelp and noticed Lilah was suddenly lame on her right hind limb. She was brought to her family veterinarian, where she received Metacam and Butorphanol prior to the collection of radiographs. Following a diagnosis of the tibial fracture, a splint and bandage were applied, and Lilah’s owner brought her to the MSU Small Animal Clinic for further evaluation.
The Orthopedics team admitted Lilah for surgery. Lilah was kept overnight in the Small Animal Intensive Care Unit, to be monitored prior to surgery the following day.
Diagnosis
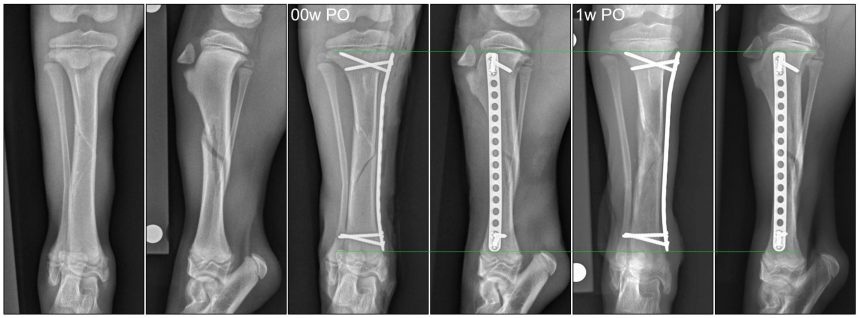
Radiographs of Lilah’s left and right tibia were performed for surgical planning. Lilah was diagnosed with a closed spiral diaphyseal fracture of the right tibia with minimal cranial displacement.
Once the diagnosis was confirmed, treatment options were discussed with Lilah’s owner (please see Comments section for more information on the treatment options).
Treatment and Outcome
Lilah was placed under general anesthesia where she underwent elastic plate osteosynthesis (EPO) using minimally invasive techniques. Post-operative radiographs confirmed good limb alignment and implant placement, and recovery from general anesthesia was uneventful.
Lilah was discharged the following day with Trazadone, Gabapentin, and Meloxicam. She was given strict activity restrictions until her radiographic recheck, as well as for instructions on incision care. Due to Lilah’s young age, she was expected to heal quickly, so a recheck appointment was scheduled for 7 days later.
Lilah returned to the MSU Orthopedic Surgery Service on November 25, 2020. Lilah’s owner reported that she had been doing well at home and noted that Lilah had been using her surgical limb more with each passing day.
On presentation, Lilah ambulated well with only a mild residual right hind limb lameness, which was expected given that surgery was performed only 7 days prior. Lilah was comfortable with limb palpation and she had a normal range of motion of all joints.
Right tibial radiographs revealed bridging callus on the lateral, cranial, and caudal cortices of the spiral fracture line, consistent with a clinical union of the fracture. The 1.5/2.0mm Veterinary Cuttable Plate (VCP) and screws were unchanged, but axial limb growth was noted from the previous radiographs, indicating that Lilah was continuing to grow normally.
Comments
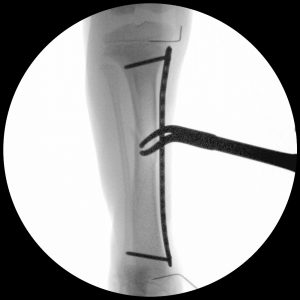
A minimally invasive approach was used for Lilah’s fracture repair, with remote incisions located at the top and bottom of the bone where the screws were placed. The fracture site was left undisturbed, allowing the fracture hematoma and tibial blood supply to remain intact, which has been shown to aid in healing. This approach was made easier by the fact that the fracture was minimally displaced. In surgery, a clamp was placed percutaneously to bring the fracture pieces closer together, and intraoperative x-rays (fluoroscopy) were taken to locate and mark the physes. It is important that surgeons ensure screws are not placed across the physes nor bridging the physes, or growth can be inhibited. In the fluoroscopic images included in this case study, needles placed into the physes during surgery as a guide can be seen.
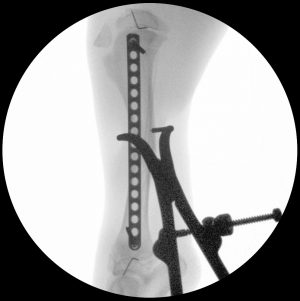
A form of fixation referred to as elastic plate osteosynthesis (EPO) was employed for fracture repair. With this technique, a less robust plate is used to bridge the fracture, spanning the length of the bone. This allows for a more compliant fixation, which in turn, allows for a reduction in 1) the force placed on the screws because the elasticity of the plate is increased, and 2) the interfragmentary strain at the fracture site because the plate is allowed to deform within the elastic limit of the metal, due to the longer working length (space between the innermost screws). Additionally, the screws are placed in a diverging fashion to minimize the risk of screw pullout, a potential complication in the juvenile bone resulting from poor material properties (softness). This technique is used in young patients because they are expected to heal very quickly, which is why an undersized implant is an acceptable fixation. As with all surgical procedures, case selection is paramount, and these techniques are not suitable for all patients.